Improving Outcomes for Patients with Cutaneous Ulcerations in the Setting of Critical Limb Ischemia, Diabetes Mellitus and Mixed Connective Tissue Disease
artassistdevice.jpg
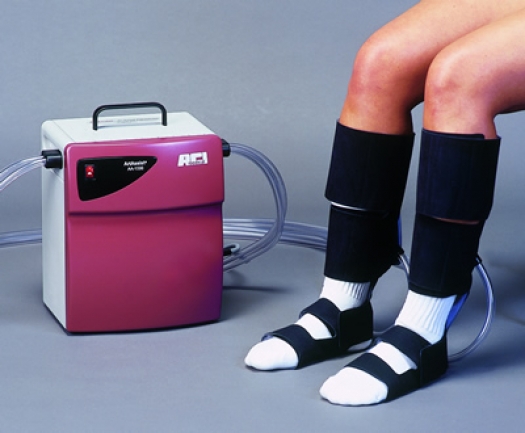
Image courtesy of ACI Medical.
Intermittent pneumatic compression (IPC) of the lower limb is a well-documented method of arterial leg inflow enhancement in patients with peripheral arterial disease (PAD). The mechanism of action parallels the natural muscular contraction of the leg stimulating blood flow. There are three very short compression cycle per minute inflating a cuff encompassing the legs and or feet simulating the beneficial effects of walking. The rapid rise of the cuff pressure assists with emptying of the venous blood of the extremities and allows oxygenated blood to move down the limb delivering nutrients to deprived tissues. This simple mechanism of action also allows edema or swelling of the extremity to be relieved. By relieving swelling, additional oxygenated blood can be delivered to the ischemic limb. Additionally, there is an increase release of nitric oxide and certain tissue and platelet derived growth factors. The nitric oxide has a positive effect on the internal cells that line the vessel wall, enabling relaxation and improved flow. Other tissue and growth factors lead to the development of new blood vessels and therefore, improve the delivery of additional oxygen and nutrients to the extremity.
Intermittent Pneumatic Compression was introduced in the medical literature as early as the mid 1930s. For almost four decades clinical interest in this method remained dormant. In the late 1970s, the delivery of pneumatic compression to the foot and ankle was reported to enhance perfusion in the skin and muscle of the leg. In 2000, Drs. Kostantinos Delis and Andrew Nicolaides began to publish their work (J Vasc Surg. 2000; 31:650-651) on intermittent pneumatic compression of the lower extremity. They found by using IPC to the foot, there was a significant improvement to the walking ability of patients with stable intermittent arterial claudication of the legs, exhibiting severe cramp-like pain of the legs. Following this study they published numerous peer reviewed medical papers on the efficacy of IPC in peripheral arterial and venous disease. There was significant advancement to the mechanism of action and understanding of the physiology associated with IPC in patients with peripheral vascular disease. Patients with intermittent claudication (IC) improved significantly with the use of IPC, their quality of life was augmented. This led to utilization in patients with ischemic pain of increased severity and outcomes also were impressive.
In November 2001, Dr. Paul van Bemmelen et al. published their work on limb salvage utilizing IPC in patients unsuitable for surgical revascularization (Arch Surg. 2001; 136: 1280-1285). This was a case series of 14 consecutive ischemic patients with IPC treatment in the setting of severe vascular disease that was not amenable to further surgery. After 3 month of treatment, 9/14 legs were saved from amputation. Patients used the IPC for 3 hours per day. This study was done at the Veterans Administration Medical Center in Northport, NY.
Drs. Victor Montori, Steven Kavros , et al. published a large study (Inter Angiology. 2002; 21: 360-366) of 107 patients with nonhealing foot ulcers and chronic critical limb ischemia with the use of IPC. In this Mayo Clinic study from 1998 to 2000, 25% of the patients had a history of lower extremity amputation, 64% had diabetes mellitus and all had peripheral arterial disease diagnosed with values well below the required levels to heal a wound. With the use of the IPC in conjunction with continued standard of care for their ischemic wounds, complete wound healing and limb preservation was achieved in 40% of the patients with chronic critical limb ischemia (CCLI) and 48% in patients with CCLI and diabetes mellitus. It should be noted that these patients had transcutaneous oxygen levels (TcPO2) significantly below the threshold for healing of wounds. In fact, patients were at the level (<20 mmHg) where wound healing was not even entertained and most patients went on to amputation.
Upper extremity digital ulceration due to ischemia occurs as a complication of scleroderma, mix-connective tissue disease and vasculitis. In 2005, Drs. David Pfizenmaier, Steven Kavros, et al published their work utilizing IPC for the treatment of upper extremity ulcers (Angiology. 2005; 56: 417-422). Based on the Mayo Clinic Vascular Center experience, more than half of these ulcers fail to heal with standard medical therapies. Digital amputation is usually required for control of pain and infection and has been advocated as the initial treatment of choice. Our results of 26 patients with 27 ischemic upper extremity ulcerations were extremely impressive. Twenty-six of 27 upper extremity ulcers (96%) healed after the use of IPC pump. One digit required amputation. The mean time to wound heal was 19 weeks when one outlier was removed. Pain reduction was significant with the use of the IPC and frequently, their use of narcotic medication was greatly reduced and or stopped with the IPC therapy.
A landmark study at Mayo Clinic with the use of IPC for improving surgical outcomes with respect to lower extremity amputation prevention was published 2008. Drs. Steven Kavros, Kostantinos Delis et al (J Vasc Surg. 2008; 47:543-549) enhanced limb preservation with the use of IPC in a controlled study with 18-month follow up. Twenty-four patients in the IPC group and control groups respectively were evaluated with the comorbidity of CCLI with foot and leg ulcers, severe ankle brachial indices and TcPO2 values. All patients were not amenable to surgical reconstruction of their arterial disease. According to standard of care practice, all patients had severe PAD and were slated for below knee amputation (BKA). It was the physician investigators impression that by using the IPC, patients could have a lesser amputation (toe, metatarsal, forefoot), utilizing the IPC during the healing phase to avoid a BKA. The results of the IPC group demonstrated 58% success with a lesser amputation and avoiding a BKA. In the control group 83% had a lesser foot amputation, failed to heal, and went on to a BKA. All patients were followed for 18 months prior to publication.
Research and patient care with the use of IPC in the arena of peripheral arterial disease continues. This is a valued medical therapy that has significant value in many areas of upper and lower extremity vascular disease. ACI Medical, Inc. (ArtAssist device) and Aircast (ArterialFlow device) are the valued pneumatic compressive devices that administer the intermittent compression therapy (IPC). These two companies have the technology that has been medically proven to deliver the required physiologic rapid rise compression that is effective for PAD. These pneumatic compression devices are small, portable, safe and easy to operate at home.
For more information regarding the ArtAssist device by ACI Medical, go to ACI Medical website and for the ArterialFlow device by Aircast, go to DJP Global.
References
Delis KT, Nicolaides AN. Improving walking ability and ankle brachial pressure indicies in symptomatic peripheral vascular disease with intermittent pneumatic foot compression: A prospective controlled study with one-year follow-up. J Vasc Surg 2000; 31: 650-661.
Delis KT, Nicolaides AN. Effect of Intermittent Pneumatic Compression of Foot and Calf on Walking Distance, Hemodynamics, and Quality of Life in Patients with Arterial Claudication. Annuals of Surgery 2005; 241: 431-441.
Van Bemmelem PS, Gitlitz DB, Faruqi RM, Weiss-Omanni J, Brunett VA, Giron F, Ricotta JJ. Limb Salvage ‘using High-Pressure Intermittent Compression Arterial Assist Device in Cases Unsuitable for Surgical Revascularization. Archives of Surgery 2001; 136: 1280-1285.
Montori VM, Kavros SJ, Walsh EE, Rooke, TW. Intermittent Compression Pump for Nonhealing Wounds in Patients with Limb Ischemia. The Mayo Clinic Experience (1998-200). International Angiology 2002; 21; 360-366.
Pfizenmaier DH, Kavros SJ, Liedl DA, Cooper LT. Use of Intermittent Pneumatic Compression for Treatment of Upper Extremity Vascular Ulcers. Angiology 2005; 56: 417-422
Kavros SJ, Dekis KT, Turner NS, Voll AE, Liedl DA, Gloviczki P, Rooke TW. Improving Limb Salvage in Critical Limb Ischemia with Intermittent Pneumatic Compression: A Controlled study with 18-month follow-up. J Vasc Surg 2008; 47: 543-549.


